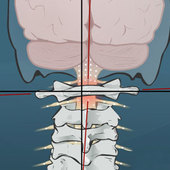
While a catastrophic injury to the CCJ often results in death, less severe injury can still result in very significant long-term consequences. From car accidents to concussions to a simple slip on the ice, the upper neck is particularly susceptible to injury. Damage to the extremely important CCJ creates a progressive, degenerative condition in the body that, once recognized, can often be successfully managed with appropriate care.
Injury to the vital and complex CCJ can have particularly devastating chronic health consequences due to the intimate relationship of this region with the neurologically crucial cervicomedullary junction. Due to this relationship, the influence of non-catastrophic injury to the CCJ on human health and quality of life is significant and evidence continues to accumulate. Whether from genetic or acquired morphological imbalances, an acceleration/deceleration injury, or the injurious forces involved in a mild traumatic brain injury, the influence of low- and high-grade lesions to the CCJ may contribute substantially to cerebrospinal fluid (CSF) flow compromise through abnormal CSF hydrodynamics as well as to dural and/or spinal cord tension/tethering.
The vulnerable neurological tissue within the CCJ is protected by sophisticated structural associations between the skull, atlas (C1), axis (C2), and root (C3) allowing for the substantial mobility of the upper neck. It is, for this reason that intervention within this ‘no-go zone’ needs to be undertaken with appropriate precautions and specificity.
Misalignments resulting from non-catastrophic sprains to the ligaments and strains to the muscles of the CCJ can be challenging for clinicians to effectively correct and stabilize. Typically, we find that the normal coupled motion capacity at the CCJ has been compromised in presenting patients.
One area that is particularly affected by structural stress in this region is the reticular formation located in the caudal brainstem. In addition to having areas such as the crucial Locus Coeruleus that control stress, pain, and panic responses, the reticular formation also has control over posture and other autonomic functions. It is for this reason that the primary objective assessment performed by the Vital Posture™ Clinic is a specific, quantifiable postural assessment.
A major sign that there may be a problem at the CCJ is a breakdown in posture. The eyes relate us to the world, the vestibular system relates our head to gravity, and our neck relates our body’s position to the head.
Simple signs to look for in your patients to see if they may benefit from an evaluation:
- Head tilt
- Unleveled shoulders and pelvis
- Twisting in the body framework
- A functionally long/short leg
Other co-morbidities and morphological imbalances that increase stress in the CCJ are:
- Platybasia & Basilar Invagination
- Atlas Assimilation or Hypoplasia
- Chiari Malformation
- Klippel-Feil Malformation
- Rheumatoid Arthritis and Trisomy 21
Due to the complexity of the biomechanics at the CCJ, a specialized approach is required to address issues arising in this region. Chiropractic craniocervical junction procedures allow for an in-depth analysis of the joint articulations at the CCJ and calculation of a specific adjusting vector that is used to realign the head and neck to reduce stress on the nervous system.
Common symptoms associated with CCJ injury are headaches, neck stiffness, pain and disability, temporomandibular joint dysfunction (TMD), and mid to lower back pain without clear pathoanatomic diagnosis. Neurological or cognitive impairments may also occur such as cervicogenic dizziness, otalgia, tinnitus, dysphagia, extremity dysfunction (coordination issues, pain), coordination challenges, sleep difficulty, and/or brain fog.
Our team works with people that need interventions at the CCJ due to:
- Chronic Post Traumatic Cervicogenic Cephalgia
- Atlantoaxial Rotatory Misalignment – Malrotation of C1 and C2
- Dural & Cord Tension
- Chronic Whiplash: Acute Acceleration/Deceleration Injury
- Post-Concussion Syndrome
- Cervicomedullary Junction Injury or Abnormality
- Cerebrospinal Fluid Flow Compromise – Abnormal CSF Hydrodynamics
- Craniocervical Instability
- Chronic Ligamentous Instability
Click for more on Request Information, Our Procedure or Patient Care